
Gestational Diabetes: What Happens Next?
Your glucose screening test came back outside of the normal range. This does not mean you’ve failed or that something is wrong with you. It does mean your body needs additional support managing blood sugar during pregnancy.
The good news: Most women can successfully manage gestational diabetes with focused nutrition, movement, and consistent monitoring.
Now we get to work!
Step 1: Support Your Blood Sugar
We recommend starting the following supplements:
Daily Supplements
Zazzee Inositol Powder – 1 scoop twice daily (increase to 2 scoops twice daily if more support is needed)
D3 + K2 (5000 IU) – twice in the morning and twice in the evening
Choose ONE of the following:
Shaklee Glucose Regulation Complex – 2–3 capsules daily with meals
(Do NOT take on an empty stomach)
OR
Chromium Picolinate (200 mcg) – with each large meal
These nutrients work together to support insulin sensitivity and healthy cellular blood sugar utilization.
If you have questions about tolerability, medication interactions, or underlying conditions, please ask before starting.


Nutrition
Step 2: Your Nutrition Must Change
This is the most important piece. We understand this can feel overwhelming. But this is temporary, and it is manageable! We highly recommend purchasing or borrowing “Real Food For Gestational Diabetes” eBook Amazon Book We carry a few copies in our lending library, along with a few other GDM cookbooks.
Recommended Dietary Pattern
The most effective frameworks we’ve seen:
Paleo-style eating
Mediterranean-style eating
These emphasize:
Protein
Healthy fats
Vegetables
Fiber
Controlled complex carbohydrates
You can find meal ideas on Pinterest by searching:
“Gestational diabetes meal plan”
“Mediterranean pregnancy meals”
“Paleo pregnancy meals”
Carbohydrate Guidelines
Minimum: 125 grams per day
Maximum: 200 grams per day
Do NOT exceed 200g/day
If you are meeting your calorie goals (see below), you should naturally meet your carb minimum.
Daily Calorie Goal
Take your body weight and add a zero.
Then add 200–400 calories depending on body size.
Example:
180 lbs → 1800 + 400 = 2200 calories/day
Undereating can worsen blood sugar instability.
Absolutely Avoid
White flour products (hamburger buns, tortillas, pizza crust)
White rice
White pasta
White sugar
Processed sweets
Breakfast cereal
Sugary drinks
Breakfast Rule
Start your day with high protein and no simple carbs.
Examples:
Eggs + avocado
Greek yogurt + nuts
Leftover dinner protein + vegetables
No cereal. No toast alone. No fruit-only breakfasts.
If you’d like a referral to a nutritionist (many insurance companies do cover this) please let us know. If you have WIC let your midwives know.


Exercise
Step 3: Exercise is Not Optional
Movement significantly improves insulin sensitivity.
You need:
Minimum 30 minutes
At least 5 days per week
This can include:
Brisk walking
Strength training
Classes
Gym workouts
We often see improved fasting numbers when women exercise in the early evening after dinner.
If you are currently sedentary, start gradually but consistently.
Blood Sugar Monitoring Instructions
This step is critical.
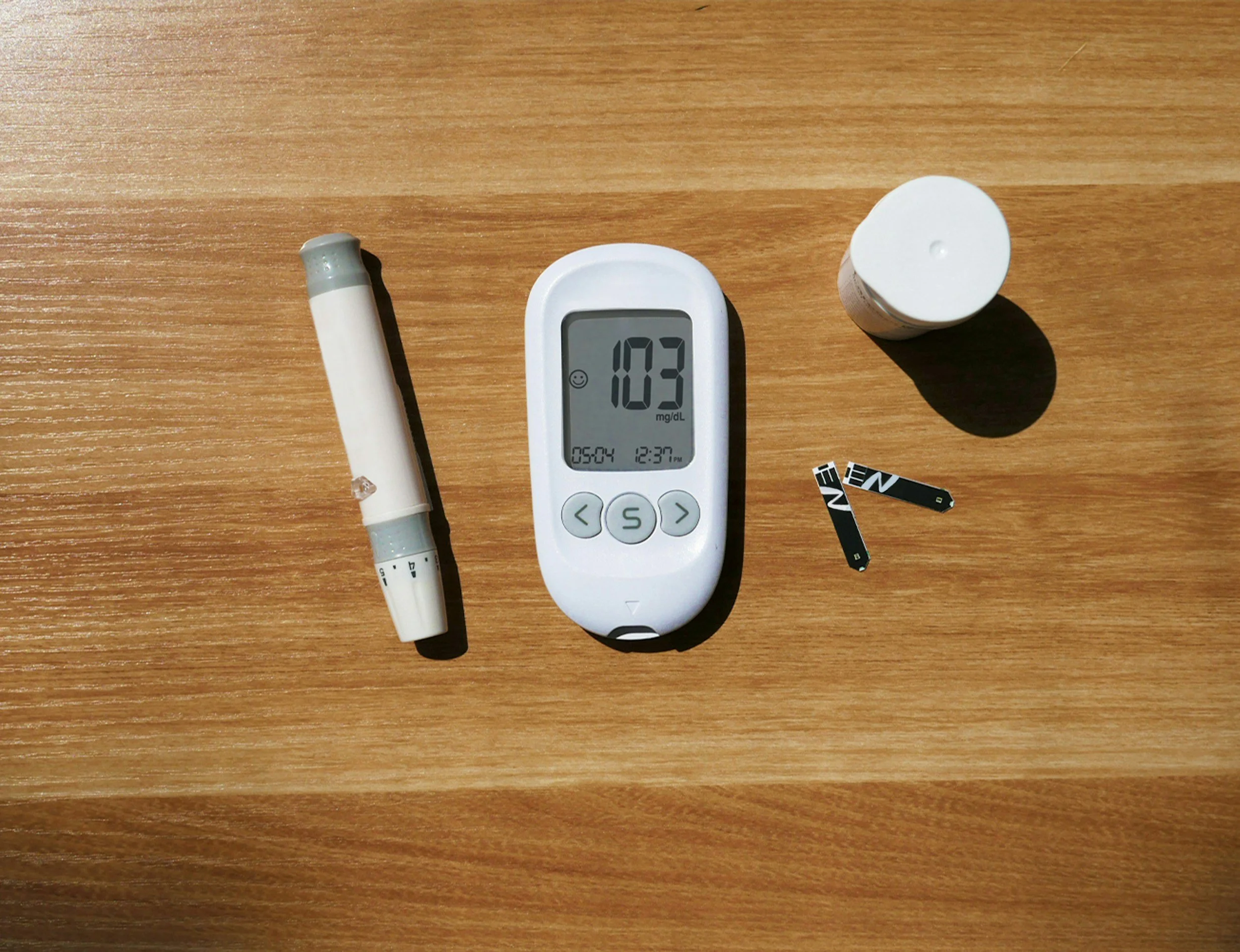
You will need to purchase a glucometer from your local pharmacy.
Test Every Day:
Fasting – First thing in the morning before getting out of bed
1 hour EXACTLY after your three largest meals
Important:
Do not eat or drink anything besides water before testing.
Timing matters. Set a timer if needed.
Snack Documentation
In the “snacks” section of your log, only document snacks eaten after your dinner post-meal reading.
This helps us evaluate what may be affecting your fasting number the next morning.
Do Not Miss Readings
Consistency determines whether you can remain under midwifery care.
You must:
Log food eaten
Log exact time of meal
Log exact time of 1-hour reading
Include sauces, creamers, milks, condiments
Be precise.
Target Glucose Ranges
Fasting: 70–90 mg/dL
1 Hour Post-Meal: 100–130 mg/dL
If you are slightly above or below, we will adjust nutrition first.
When to Call
140–180 mg/dL: Log it
≥180 mg/dL or concerning pattern → Call office during business hours
≥200 mg/dL OR symptoms (nausea, vomiting, headache, excessive thirst, frequent urination, confusion) → Call the on-call line:
817-477-6551
Weekly Submission Requirement
Every Friday:
Upload your COMPLETED LOG in your Maternity Neighborhood Messages or email hello@dfwcommunitybirths.coom
Failure to submit logs may affect your eligibility to remain in midwifery care.
Bring your glucometer to every prenatal visit.
Can I still have an Out of Hospital Birth?
Most women successfully manage gestational diabetes with nutrition and lifestyle changes alone.
According to the reference guide Your Quick Guide to Gestational Diabetes & Insulin Resistance, approximately 85% of women can control blood sugar through diet and lifestyle measures.
If blood sugars remain uncontrolled despite intervention, we may need to discuss collaborative or transfer care for safety.
Our goal is always:
Healthy mother
Healthy baby
Appropriate risk level for out-of-hospital birth
Remember, give yourself grace!
Gestational diabetes develops because of placental hormones that create insulin resistance. This is not a personal failure!
However, unmanaged blood sugar increases risks including:
Macrosomia
Shoulder dystocia
Neonatal hypoglycemia
Increased cesarean risk
This is why we take monitoring seriously.
For additional evidence regarding induction and gestational diabetes, see:
https://evidencebasedbirth.com/evidence-on-induction-for-gestational-diabetes/
You Can Do This!!
This is a season.
It requires discipline.
It protects your baby.
We will walk this with you, but the daily work is yours.
If you have questions about:
Supplements
Meal planning
Exercise ideas
Concerning readings
Reach out.
We are here to support you.
Please read this Informed Choice and Consent GDM document which we will have you sign at your next appointment

